Restless Leg Syndrome
Definition
Restless leg syndrome (RLS) is a common sleep-related movement disorder marked by an uncomfortable urge to move the legs that occurs during periods of inactivity, especially in the evenings, and is transiently relieved by movement.
Causes
Although the pathophysiologic basis has yet to be fully understood, there are several correlates that have been found. Neurodegeneration has not been implicated, however, there are a few CNS correlates to include:
Common risk factors for RLS include:
• Family history of RLS
• Low iron stores
• Uremia (Chronic kidney disease)
• Neuropathy
• Spinal cord disease/trauma
• Pregnancy
• Multiple Sclerosis
• Parkinson’s Disease
Symptoms and Clinical Signs
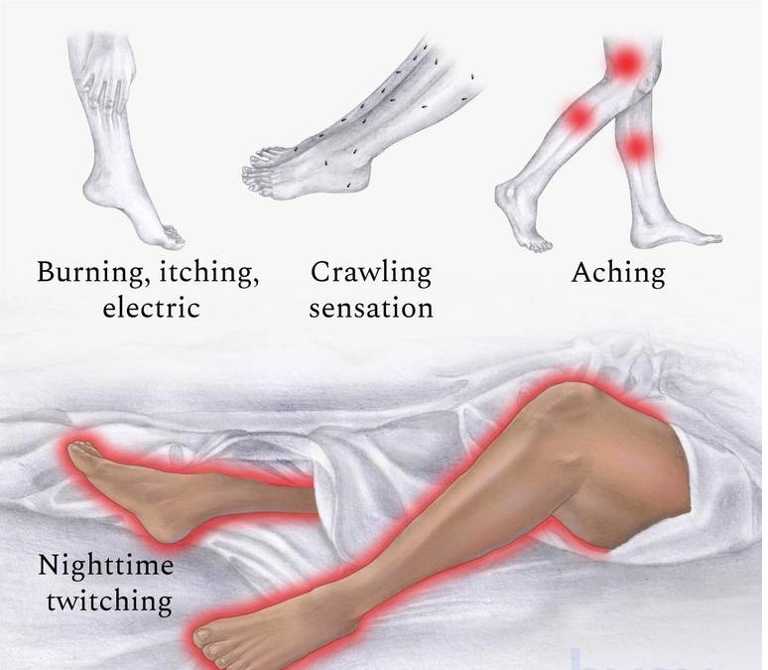
The hallmark symptom is an uncomfortable ache or tension deep in the calf muscles with an urge to move the legs with a kick or repetitive motion. Symptoms usually present in the evenings when the patient is lying down to sleep or during other periods of rest. Transient symptomatic improvement can be achieved by walking, stretching, massage, or by applying heat or cold presses. RLS may exacerbate or precipitate other disorders such as insomnia, depression, or anxiety. Sleep partners may report leg movements while the patient is asleep. Patients may find that medications including antihistamines (especially 1st generation), dopamine receptor antagonists, and select antidepressants worsen or even cause their RLS symptoms
Diagnosing RLS
Restless Leg Syndrome is a clinical diagnosis requiring all five of the following clinical features.
1. An urge to move the legs, often accompanied or caused by uncomfortable sensations in the legs.
2. Symptoms begin or worsen during periods of inactivity such as lying or sitting.
3. Uncomfortable features are relieved by movement, such as walking or stretching as long as the activity continues.
4. Symptoms are worse in the evening.
5. Symptoms are not accounted for by another medical or behavioral condition
Treatment
Iron replacement therapy has shown mixed results for efficacy in trials and should only be initiated in patients whose fasting serum ferritin levels are below 75ng/mL. Nonpharmacologic therapies have been shown to be effective in mild cases of RLS and have been shown to help reduce the medication requirements in severe cases.
These therapies include behavioral strategies such as:
• Mental alerting techniques during times of rest
Avoidance of aggravating factors such as
▪ Neuroleptics
▪ Dopamine-blocking antiemetics
▪ Sedating antihistamines
• Regular exercise
• Reduce caffeine intake
Go Back Restless leg syndrome (RLS) is a common sleep-related movement disorder marked by an uncomfortable urge to move the legs that occurs during periods of inactivity, especially in the evenings, and is transiently relieved by movement.
Causes
Although the pathophysiologic basis has yet to be fully understood, there are several correlates that have been found. Neurodegeneration has not been implicated, however, there are a few CNS correlates to include:
- Reduced CNS Iron stores
- Increased CNS Dopamine metabolism
- Other neurotransmitter abnormalities (endogenous opioids, glutamate, glutamine, adenosine, histamine, and gamma-aminobutyric acid (GABA)
- Resting state CNS network connectivity disorders between: Thalamus, Pons, Red nucleus, and Brainstem
- Afferent nerve central sensitization leading to hyperalgesic neuropathic pain
- Abnormalities of microvascular function in the legs (altered leg intramuscular blood flow, peripheral hypoxia, and reduced endothelial function)
Common risk factors for RLS include:
• Family history of RLS
• Low iron stores
• Uremia (Chronic kidney disease)
• Neuropathy
• Spinal cord disease/trauma
• Pregnancy
• Multiple Sclerosis
• Parkinson’s Disease
Symptoms and Clinical Signs
The hallmark symptom is an uncomfortable ache or tension deep in the calf muscles with an urge to move the legs with a kick or repetitive motion. Symptoms usually present in the evenings when the patient is lying down to sleep or during other periods of rest. Transient symptomatic improvement can be achieved by walking, stretching, massage, or by applying heat or cold presses. RLS may exacerbate or precipitate other disorders such as insomnia, depression, or anxiety. Sleep partners may report leg movements while the patient is asleep. Patients may find that medications including antihistamines (especially 1st generation), dopamine receptor antagonists, and select antidepressants worsen or even cause their RLS symptoms
Diagnosing RLS
Restless Leg Syndrome is a clinical diagnosis requiring all five of the following clinical features.
1. An urge to move the legs, often accompanied or caused by uncomfortable sensations in the legs.
2. Symptoms begin or worsen during periods of inactivity such as lying or sitting.
3. Uncomfortable features are relieved by movement, such as walking or stretching as long as the activity continues.
4. Symptoms are worse in the evening.
5. Symptoms are not accounted for by another medical or behavioral condition
Treatment
Iron replacement therapy has shown mixed results for efficacy in trials and should only be initiated in patients whose fasting serum ferritin levels are below 75ng/mL. Nonpharmacologic therapies have been shown to be effective in mild cases of RLS and have been shown to help reduce the medication requirements in severe cases.
These therapies include behavioral strategies such as:
• Mental alerting techniques during times of rest
Avoidance of aggravating factors such as
- Sleep deprivation
- Precipitating medications
▪ Neuroleptics
▪ Dopamine-blocking antiemetics
▪ Sedating antihistamines
• Regular exercise
• Reduce caffeine intake